‘I was losing A LOT of hair, barely sleeping and feeling anxious and exhausted all the time. My family could hardly recognize me, and I felt like a stranger in my skin. I have always been a very calm person, even under pressure. However, when I finally decided to seek support, the mere thought of driving my kids to school almost gave me a panic attack. After an extensive ‘health interview,’ it turned out that my adrenal glands were part of my issue and thorough testing (which conventional doctors refused to do), revealed that I had adrenal fatigue. I was stunned and outraged! No one had ever said anything about my adrenal glands!’

This story is just one real case scenario of one of my patients (Angie K., 33). However, there are (too) many of you out there who suffer from similar symptoms and are at a loss as to how to deal with how they feel. So, in this article, I’ll cover the basics of ‘adrenal fatigue,’ the most popular myths associated with it and how to treat it naturally.
What exactly are the adrenal glands?
Also known as the suprarenal glands, the adrenal glands lie just on top of the kidneys. These little glands have a flat pyramidal shape and weigh only 3.5 to 5g! Along with the hypothalamus and the pituitary gland, the adrenal glands control our energy, metabolism, and hormonal balance. Together, they form part of the Hypothalamus Pituitary Adrenal (HPA) axis.
The adrenal glands consist of:
(i) The adrenal cortex which is subdivided into three zones, each of which secretes different hormones namely:
– The mineralocorticoids which are involved in mineral balance. Aldosterone is the principal mineralocorticoid produced by the adrenal glands – this hormone plays a crucial role in the regulation of blood pressure.
– The glucocorticoids which affect glucose homeostasis (blood sugar control), metabolism and regulate resistance to stress. These include cortisol (hydrocortisone), corticosterone and cortisone.
– The androgens which are steroid hormones that exert masculinizing effects. The major androgen secreted by the adrenal gland is dehydroepiandrosterone (DHEA).
(ii) The adrenal medulla which produces three catecholamine hormones namely norepinephrine, epinephrine, and dopamine.
As you can see, the adrenal glands are master regulators that, not only crank out 57 different hormones but also manage how other hormones work!
[color-box color=”main”]Did you know?
In women, these androgens promote libido (sex drive) and are converted into estrogens (feminizing sex steroids) by other body tissues. However, after puberty in males, the androgen testosterone is released in much larger quantities – these render the effects of adrenal androgens insignificant.[/color-box]
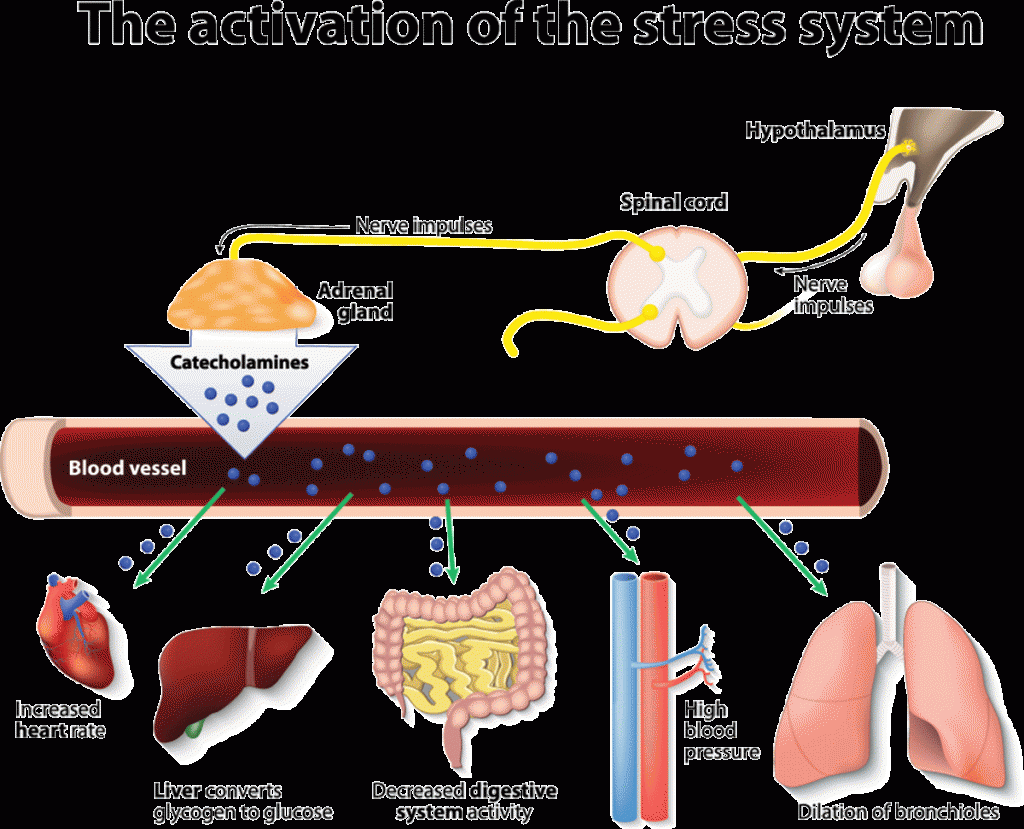
What’s the link between the adrenal glands and stress control?
The HPA axis acts as a feedback loop: in a nutshell, when you’re stressed, the hypothalamus will release Corticotropin Releasing Hormone (CRH) which signals the pituitary gland to release Adrenocorticotropic Hormone (ACTH).
This ACTH then ‘tells’ the adrenal glands to release cortisol, the ‘fight-or-flight’ hormone, which will then:
- Promote the release of sugar into the blood (as a means to create a burst of energy that will help the body deal with the stressor).
- Suppress the digestive and reproductive systems and lower immune system responses (so as to direct all the energy available to either fighting or fleeing.
Once the stressor is gone, negative feedback cycles turn off the HPA axis – this stops cortisol release.
Now that you know what the adrenal glands are and how they function; let’s tackle the first myth.
Myth 1: The adrenal glands get fatigued.
Let set the record straight: the adrenal glands don’t get tired. They don’t burn out. They don’t stop working. They don’t collapse.
You see, the term ‘adrenal fatigue’ is utilized only to make the concept of adrenal dysfunction easier to grasp – it refers to a collection of symptoms and is not a disease. However, the issue with this term is that it gives the impression that the adrenals are unable to produce enough hormones. There are some health conditions where the adrenals cannot make enough hormones – these include Cushing’s syndrome (an excess of cortisol in the blood) and Addison’s disease (primary adrenal insufficiency). However, adrenal fatigue is completely different from these health issues.
In adrenal fatigue, the adrenals are still making cortisol, and it is highly likely that routine cortisol tests will show that your cortisol is within the normal range since that range was designed to diagnose Cushing’s syndrome or Addison’s disease.
And the problem is that most conventional doctors equate adrenal dysfunction to either of these life-threatening diseases. So if you tell these doctors that you have adrenal fatigue, they’ll probably look at you like you have two heads and probably tell you that your symptoms are ‘all in your head.’
So what exactly is ‘adrenal fatigue’?
![Fig. 1. A simplified schematic representation of the central and peripheral components of the stress system, their functional interrelations and their relations to other central systems involved in the stress response. The CRH/ AVP neurons and central catecholaminergic neurons of the LC/NE system reciprocally innervate and activate each other. The HPA axis is controlled by several feedback loops that tend to normalize the time-integrated secretion of cortisol, yet glucocorticoids stimulate the fear centers in the amygdala. Activation of the HPA axis leads to suppression of the GH/IGF- 1, LH/testosterone/E2 and TSH/T3 axes; activation of the sympathetic system increases IL-6 secretion. Solid lines indicate stimulation; dashed lines indicate inhibition. (Adapted from Chrousos and Gold [1]).](https://www.researchgate.net/profile/George_Chrousos/publication/11083444/figure/fig1/AS:277058686078983@1443067346853/Fig-1-A-simplified-schematic-representation-of-the-central-and-peripheral-components-of.png)
However, some individuals can become unable to properly habituate to the daily stress they face, especially if that stress is more significant than simply being stuck in a traffic jam on the way to work.
Think of stressors like:
- Consistently not getting enough quality sleep
- Shift work
- Eating a diet that revolves around processed foods
- Not consuming enough nutrients (even though you may be eating a Paleo diet)
- Poor gut health
- Chronic disease
- Facing serious financial issues
- Caring for a sick relative
- Being in an abusive relationship
- Overtraining
So, each time these individuals face their stressor, they activate their HPA axis, marking the start of the stress response. Eventually, as the adrenals keep pumping out more and more cortisol, the body becomes less sensitive to it, and a state of cortisol resistance develops, marking the debut of HPA axis dysfunction. Instead of only turning on during acute stress and turning off once the stressor goes away, the HPA axis is constantly activated until the mechanisms that switch it off stop working.
When this happens, cortisol levels will be high because the body is continuously producing the hormone.
However, at some point, the HPA axis will not be able to keep up, and cortisol levels will start declining until they become too low. So, as you can see, the problem is with the HPA axis, not with the adrenal glands per se.
Note: The term ‘adrenal fatigue’ is used throughout this post because very few people are aware that adrenal fatigue is not real. As such, not many readers would search for ‘HPA axis dysfunction.’
[color-box color=”main”]Bottom line: Want to talk to your doctor about ‘adrenal fatigue’? Then use the term Hypothalamic Pituitary Adrenal (HPA) axis dysfunction, maladaptation or dysregulation.[/color-box]
What are the symptoms of adrenal fatigue?
Cortisol is not the villain here – as explained earlier, it plays crucial roles in the body. While HPA axis dysfunction is not life-threatening, the symptoms it causes can prevent you from living the life you deserve. The most common symptoms are listed below:
- Fatigue, lethargy
- Depression
- Irritability
- Anxiety
- Panic attacks
- Brain fog, trouble focusing on stuff
- Being unable to handle stress
- Waking up tired but being unable to sleep at night (tired but wired)
- Feeling exhausted between 3 and 5om
- Low blood pressure
- Heart palpitations
- Hair loss
- Low blood sugar
- Sugar cravings
- Constipation and/or diarrhea
- Cold hands and feet
- Low thyroid function
One of the things I have noticed in patients with adrenal fatigue is that they will often experience something at a similar time of the day, almost every day. For instance, some may experience an energy crash at around 2 pm while others may wake up every day at 3 am with their mind racing. If that’s your case, this may indicate an issue with your cortisol levels since this hormone also has its daily rhythm.
[color-box color=”main”]Bottom line: The symptoms of adrenal fatigue vary tremendously between individuals. So make sure to get tested.[/color-box]
How to test for Adrenal fatigue
You can check your cortisol levels through:
- Blood/serum cortisol tests carried out around 8 am. The optimal range for adults is 10-15 μg/dL.
- Salivary 4-point cortisol test which is carried out usually before breakfast, lunch, dinner, and bedtime so as to assess the cortisol slope.
- Dried urine hormone testing (currently the most accurate testing method).
Understanding how to interpret those tests is beyond the scope of this article. So make sure to work with a functional medicine practitioner.
Myth 2: Adrenal fatigue isn’t that serious.
HPA axis dysfunction occurs in three stages:
- Stage 1: Cortisol levels would usually be elevated throughout the day so you might feel stressed out, find it hard to sit still and unable to sleep at night.
- Stage 2: In this stage, you’ll start showing signs of cortisol depletion such as brain fog, low energy levels, and a reduced ability to handle stress as well as blood sugar imbalances that can make you cranky if you miss a meal.
- Stage 3: If you reach this stage, you’ll experience all the symptoms of stage 2 but to a higher degree.
As you can see, if left unchecked, HPA axis dysfunction can actually worsen. In fact, research suggests that HPA axis dysfunction can adversely affect the immune system as well as the body’s immune responses. In other words, failing to reset your body’s natural rhythms can lead to:
- An increased vulnerability to infectious diseases and depression.
- Higher risks of chronic diseases and certain cancers.
- Autoimmune conditions.
[color-box color=”main”]Bottom line: If you can identify with any of the above stages, please make sure to see a qualified practitioner.[/color-box]
Myth 3: Just pop some pills and your adrenals will be A-OK.
If your HPA axis is out of sync, the cure is to address the root cause(s) of this dysfunction. Simply taking ‘adrenal support’ pills may not only prove to be ineffective: that can be downright dangerous as well.
So here’s how to ensure that you’re also restoring the natural rhythm of your HPA axis:
Step 1: Review your diet.
- Ditch refined carbs – these can seriously stress the adrenals. I’m talking about any food that contains added sugar, high fructose corn syrup, wheat flour as well as any foods that contain ingredients you can’t begin to pronounce.
- Steer clear from pro-inflammatory oils such as oils of canola, cottonseed, safflower, sunflower or soybean. Try virgin coconut oil, extra virgin olive oil or grass-fed butter or clarified butter instead.
- Try to go off any caffeine-containing beverage for a few weeks since caffeine can slow down the recovery rate of the HPA axis.
- Say no to alcohol – not only can booze add undue stress on your adrenals, but it can also promote urinary nutrient losses.
- Try to consume grass-fed meat, wild fish and pastured poultry and eggs as often as you can. If these aren’t available, or you don’t have the budget for that, just make sure to discard the skin and trim as much fat as possible from the meat.
- If YOU tolerate legumes and can digest them, make sure to soak them properly for at least 24 hours before cooking. I usually advise my patients to add some vinegar to the soaking water and to change the water every 3 to 6 hours.
And make sure you’re getting enough calories, healthy fats, complex carbohydrates vitamins and minerals.

(i) Calories matter (but not in the way you may think)
Most of the patients who start my adrenal support treatment are already eating a Paleo-ish diet (I individualize the diet based on their ancestral lineage). In other words, they are eating real foods. However, many of them fail to eat sufficient calories.
[color-box color=”main”] What I usually advise my patients: What you want to do is to estimate your calorie needs – I like this calorie calculator – and then track your intake for a few days using online programs like MyFitnessPal. Using this method, I often see patients who are undereating by at least 500 calories per day. That’s a HUGE stressor for the body and is extremely nasty for adrenal health.[/color-box]

(ii) Ditch low-carb diets and enjoy more healthy fats.
Since many patients with adrenal dysfunction tend to have weight issues (either excess body weight or difficulty to maintain a healthy weight), many end up considerably decreasing their carbohydrate and fat intake.
The issue is that carbohydrates and fats both play a huge role in blood sugar control which, in turn, affects the function of the adrenals.
As mentioned earlier, the adrenal cortex produces glucocorticoids such as cortisol. This hormone increases blood sugar levels either (i) via gluconeogenesis (production of new sugar by the liver) or (ii) by counteracting the effects of insulin and preventing glucose uptake in cells so as to keep that glucose in the blood. These two actions help increase blood sugar levels when these are low.

Your blood sugar levels can drop if you’re not consuming enough carbohydrates or if your diet is too low in fat – low-fat diets tend to cause blood sugar levels to spike and then crash.
What’s the problem with low blood sugar levels? Well, your body sees it as a stressor since the brain needs a steady amount of glucose to function and because blood sugar levels that are low enough can kill you!
And since your body doesn’t want you to die, your adrenals will keep responding to drops in blood sugar levels. This will worsen HPA axis dysfunction and may exacerbate your symptoms.
[color-box color=”main”]What I usually advise my patients:
- Consume a diet that will keep blood sugar levels super steady – you can try the following percent of calories range: 20-30% of calories from carbohydrates, 20-30% of calories from proteins and 40-60% of calories from fat. IMPORTANT NOTE: Once you get an approximate picture of the amount of food you need, please don’t keep counting calories and macronutrients. Instead, try to focus on your body’s innate satiety cues.
- Eat at least three meals per day – each meal, even dinner, should contain carbohydrates, proteins, and fats.
- If your blood glucose levels drop between your main meals, try a snack such as a fruit and some coconut butter.[/color-box]

(iii) Vitamins and minerals – prioritize dietary sources first
For your adrenals to work properly, they need various nutrients including:
- Vitamin A
- Vitamin B5 – Needed to maintain the structural integrity of the adrenal glands.
- Vitamin B6 – Required for cortisol to be able to regulate blood sugar levels via gluconeogenesis. Since oral contraceptives decrease B6 levels, make sure to get enough of this B vitamin if you’re on the pill.
- Vitamin B12
- Vitamins C and D – Required for the production of adrenal hormones such as epinephrine and norepinephrine. Vitamin C levels drop each time we activate the HPA-axis.
- Magnesium – This mineral gets depleted during periods of stress.
- Omega-3 fatty acids
- Zinc – This mineral is involved in immune regulation.
- Probiotics – Your microbiome will influence the gut-brain axis.

[color-box color=”main”]What I usually advise my patients:
- Before you try supplements, make sure that your diet contains enough REAL foods such as liver, leafy greens, fruits, fermented foods, shellfish, pastured eggs and so on.
- You may benefit from supplements, but these will depend on your blood test results. For instance, many websites routinely recommend licorice root. The issue is that this herb will increase cortisol levels so if your cortisol is already high, it doesn’t make sense to take something that would increase it further, right? [/color-box]
Remember: While supplements are often necessary in cases of HPA axis dysregulation, taking the wrong supplements, or the wrong dosage of the right supplement can do more harm.
(iv) Salt things up!
HPA-axis dysfunction reduces the production of aldosterone, the hormone in charge of retaining water and sodium in order to regulate blood pressure. Simply add some non-processed table salt (such as real sea salt or Himalayan salt) to your foods and drinks.
Step 2: Review the quality of your sleep.
Do you feel tired at night but unable to fall asleep because your mind keeps going and going? Or maybe you wake up at night feeling jittery or anxious?
To promote restful sleep, here’s what you want to:
- Switch off all electronic devices at least 1 hour before bedtime. If you absolutely need to use your laptop or smartphone at night, then install f.lux (Windows or Mac), twilight (Android phones).
- Try wearing amber lensed goggles after sunset – these have been shown to improve sleep quality by blocking blue light wavelengths which suppress melatonin production. Melatonin is the hormone that helps you enjoy quality sleep.
- Eat a small snack containing carbohydrates and fats about 1 hour before you hit the hay. You could have: a fruit and almond butter or full-fat real cheese; frozen fruits with coconut cream; herbal tea with honey and a dollop of coconut cream; a small piece of sweet potato chocolate brownie. Or make some strawberry coconut ice-cream (check out the video below).
- Try magnesium glycinate about 30 minutes before going to bed – this will help you unwind and will promote restful sleep.
[color-box color=”main”]Make sure to: Get a full 8 hours of sleep every night.[/color-box]
Step 3: Review your lifestyle.
(i) Are you overly stressed?
In the world we live in, most of us cannot escape stress. However, there are things we do that put undue stress on us. For example, many women entrepreneurs I work with tell me they just don’t know how to juggle a healthy lifestyle, work and family at the same time. A review of their day often reveals that they’re trying to be a superwoman and get caught up in many administrative jobs they could delegate. Or many others get so caught up with answering emails that half of their day is gone and they haven’t even started on the important stuff they need to do.
Besides trying to reorganize your day, you could try stress-management techniques that revolve around mind-body activities. For instance, you could try Tai Chi, deep breathing, mindfulness-based stressed reduction or visualization. Try out these techniques to see what works best for what works best for YOU and practice these for 1 or 2 minutes every day – this will help retrain the HPA axis.

(ii) Do you have enough social support?
Did you know that a LOT of research now shows that the quality of our social ties has an enormous impact on our mental health? I’m not saying you should spend more time on online social networks but that you could benefit from reconnecting with your friends or family. Why not schedule a family outing or call one of your good friends. You could also volunteer at a local soup kitchen. Or you could start a group. Any activity that makes you happy will help you recover from HPA axis dysfunction.
(iii) Are you too sedentary? Or maybe you’re over-exercising?
You read that right – exercising too much can spell big trouble for the adrenals. In fact, I’ve seen many clients for whom over-exercising turned out to be the root cause of their HPA axis dysfunction – many of them had to stop exercising altogether to recover fully.
What you want to do is find a specific type and amount of exercise that makes you feel better and more energized (instead of draining you). Going for a walk every day should be okay; starting CrossFit or HIIT is probably not a good idea.

Myth 4: Intermittent fasting is safe for individuals with adrenal fatigue.
While intermittent fasting has its merits, those with adrenal fatigue should not skip breakfast if they want to recover rapidly. As mentioned the ideal diet for adrenal fatigue is one that helps you maintain your blood sugar levels because you want to minimize the amount of cortisol your body relies upon on a daily basis.
You’re already in a fasted state when you wake up in the morning and if you continue fasting; your body will need more glucose to meet its needs. It will either pull this glucose from your liver stores or create new glucose from protein fat – these two mechanisms will increase your blood levels of cortisol.
[color-box color=”main”]What I usually advise my patients:
- Try to eat a high protein and moderate carbohydrate breakfast within 30 minutes of waking up.
- Aim for 4 ounces of animal protein with some fruit and healthy fats.[/color-box]
Myth 5: You’re stuck with adrenal fatigue.
While HPA axis dysfunction is very real, you can reverse this condition by resetting your body’s natural rhythms. The first step is to implement the various tips mentioned in this article. I also strongly advise you to work with a healthcare professional so as to determine which dietary, exercise and supplement regimen will work best for you.