‘Well, whatever you do, your kidneys’ health will deteriorate. In a few years, you’ll need to start dialysis.’
Two years later, the rheumatologist’s words still resonate painfully in my ears. And the extremely brief, yet intense, look of despair in my father’s eyes will forever break my heart and make me furious at the same time.
That night, as I was driving back home from the doctor’s office, I took a deep breath and told my dad not to start the immunosuppressant prescribed by the physician. And my dad became the very first patient I walked through the autoimmune Paleo diet. Not only are his kidneys working much better but he is no longer taking any medications and has managed to lose 30cm2 of fat around his organs!
If you have an autoimmune disease, before you opt for pills, you might want to try the autoimmune Paleo lifestyle – it has done wonders for many of my patients. In this article, I will outline the protocol (diet, lifestyle and supplements) that can help you get your symptoms under remission.

Autoimmune diseases – When your body betrays you
The role of the immune system is to detect and attack foreign invaders by using antibodies to recognize specific proteins (antigens) in foreign cells. However, in some individuals, the body accidentally produces antibodies that target the body’s own cells – these are known as autoantibodies.
The good news is that the body has a natural backup system to get rid of cells that produce autoantibodies. But the unpleasant news is that, if this system fails, the immune system will be stimulated to attack, not only foreign proteins but the body’s own proteins as well. Symptoms of autoimmune diseases will start showing up once the immune system has caused enough damage to the cells.
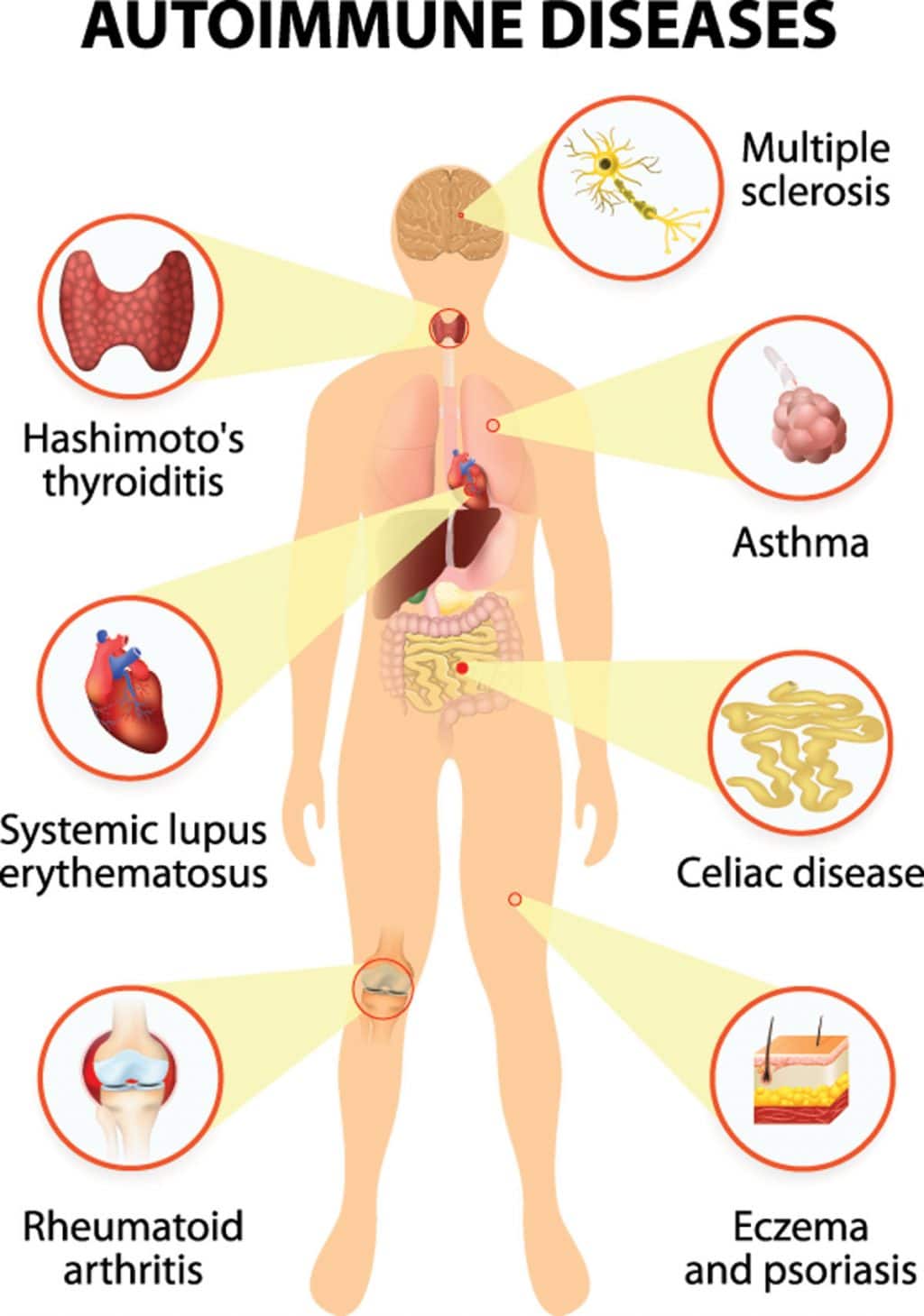
A few examples of autoimmune disease include:
- Alopecia (spot baldness)
- Arthritis – any type
- Celiac disease
- Chronic fatigue syndrome
- Eczema
- Endometriosis
- Glomerulonephritis
- Grave’s disease
- Hashimoto’s thyroiditis
- Lichen planus
- Multiple sclerosis
- Pernicious anaemia
- Psoriasis
- Systemic lupus erythematosus (SLE)
- Type 1 diabetes
- Vitiligo
You may have noticed that the above (non-exhaustive) list is very broad. Well, that’s because the nature of the autoimmune disease will depend on which proteins or cells are being attacked. For example, in arthritis, the tissues of the joints are attacked whereas, in Hashimoto’s Thyroiditis, the immune system targets the thyroid. And of course, the symptoms will vary depending on where the damage occurs.
What causes autoimmune diseases?
We still don’t know exactly why or how individuals develop these diseases but key factors include:
- A genetic susceptibility – different family members can develop various types of autoimmune disease.
- Environmental triggers – these include exposure to chemicals, heavy metals like mercury, pollutants, mycotoxins from molds, and hormones as well as different types of infections like Candida.
- Diet and lifestyle habits that increase intestinal permeability (also known as a ‘leaky gut’).
How are autoimmune diseases diagnosed?
Unfortunately, autoimmune diseases are difficult to diagnose until they have progressed to the point where the symptoms are severe, predictable and fall into a pattern that is consistent with a particular autoimmune disease. However, your medical history, physical exams, biopsies, blood tests and radiography results can help towards a diagnosis.
Tests that can help diagnose an autoimmune disorder
No single blood test can definitively determine that you have an autoimmune disease. Instead, an array of tests is usually needed. Your healthcare provider will work with you to determine which of the following tests you would benefit from doing:
- Antinuclear antibodies
- Autoantibodies
- Secretory IgA antibodies
- Complete blood count – you can also do a CBC with differential
- C-reactive protein (CRP)
- Erythrocyte sedimentation rate (ESR)
- Food sensitivities and allergies
- Hormone levels
- Deficiencies of micronutrients
- Organ function
Is there a cure for autoimmune diseases?
Short answer: No (but there’s a solution).
The truth is that, once your body has learned to attack itself, it just won’t forget how to do that. And this is why the medical establishment considers autoimmune diseases as a life sentence. So, if you see a conventional doctor, your treatment, or management protocol, will typically include:
- Hormone replacement if you have a disease which causes hormone deficiency. Examples include type 1 diabetes and hypothyroidism.
- Corticosteroids, such as prednisone, suppress the immune system. These are prescribed when the body becomes cortisol-resistant, and the immune system is in overdrive.
- Disease-modifying anti-rheumatic drugs, or DMARDs, which are often prescribed to very sick patients.
Why not simply take these medications?
Because they don’t address the root cause of your disease. These drugs only mask your symptoms but may end up causing more harm:
- Although corticosteroids can be life-saving, their main use is to relieve symptoms. While corticosteroids do reduce inflammation and immune activation, they also hinder healing. And once you get off these drugs, symptoms often come back with a vengeance as your body is now even more cortisol-resistant. Moreover, these drugs come with loads of unwanted side effects such as weight gain, appetite stimulation, sleep issues and can zap your energy levels. And all of these side effects have serious adverse effects on gut health.
- Even at low doses, DMARDs have been found to increase intestinal permeability and may cause liver injury as well as diarrhea and vomiting. Besides being linked to higher risks of infection and a greater vulnerability to developing cancer, DMARDs can also cause autoimmune diseases such as SLE, myasthenia gravis, and Lambert-Eaton myasthenic syndrome as side effects!
Important note: Do not attempt to stop these medications on your own. It is imperative that you do so under medical guidance.
 So what is the solution?
So what is the solution?
Although there is no cure for autoimmune diseases, you can stop your disease from progressing and put your symptoms into total remission for the rest of your life! Wondering how? Simple: work with a healthcare practitioner who will help you apply the principles of the autoimmune Paleo lifestyle (outlined below).
I won’t sugar-coat it
If you truly want to put your symptoms into remission, only changing what you eat will not be effective. You NEED to practice a healthy lifestyle as well.
Want to be symptom-free? Review your lifestyle.
1. Get enough quality sleep.
Did you know that not getting quality sleep for only three nights or going 40 hours without sleep can lead to increased inflammation and an overly stimulated immune system?
Oh, that’s okay, you’ll just sleep more during the weekend, and everything will be peachy… Right?
Unfortunately, no. Research indicates that pro-inflammatory cytokines remain high for at least two days after increasing sleep to nine hours a night. In other words, the ‘catching up’ won’t help your immune system recover from late nights and early mornings.
So, not getting enough sleep during the week and hibernating during the weekend will seriously mess up your immune system.
Check out this article for tips on how to improve the quality of your sleep.

2. Practice stress management methods.
I’m sure you know that being chronically stressed out can never be a good thing. But do you know why it is even more important for you to deal with your stress if you have an autoimmune disease?
In a nutshell, when you are stressed, your body responds by producing more cortisol to help you deal with your stressor. While our body is well equipped to deal with short-lived stressful situations, chronic stress can wreak havoc on the hypothalamus-pituitary-adrenal (HPA) axis – this may lead to cortisol dysregulation. When this happens, you may notice that your cortisol levels:
- Either follow a normal pattern but are chronically elevated.
- Or follow an ebb and flow pattern while still being higher than normal.

If I tell you that cortisol can open up the tight junctions between enterocytes (cells of the intestinal lining), what do you think will happen if your cortisol levels are elevated?
You’re right: chronically high levels of cortisol can increase intestinal permeability which, as mentioned earlier, is involved in the development of autoimmune disease.
Moreover, chronic stress has also been linked to a dysfunctional immune system.
Discussing stress-management techniques is beyond the scope of this article but here are a few tips that can help:
- Get some more you-time. Even if that’s just five minutes. Just take some time off to breathe in and out deeply.
- Make a list of things that stress you out. Then categorize them as things you can change and things you have no control over.
- Review your priorities – health vs. [fill this in]
- Work with a therapist.
3. Connect with your loved ones.
Did you know that physical contact, such as hugging a family member, can reduce cortisol levels by decreasing the activity of the HPA axis? Plus touching someone you love also increases the ‘love hormone’ oxytocin which can improve your immune function!
The important point here is that you need to feel connected (even if that’s just your pals from the knitting group) – this will make it easier to cope with and heal from your autoimmune disease.
4. Are you taking any of the following drugs?
Before taking any medication, check the associated side effects. If possible, avoid taking drugs that may cause any type of gastrointestinal issues such as constipation, diarrhea, abdominal pain, vomiting or nausea.
The most common offenders include:
- Anti-inflammatory drugs such as ibuprofen, naproxen, and aspirin (prescribed as pain reliever)
- Immune-suppressing drugs like corticosteroids and DMARDs
- Acid-suppressing drugs such as proton pump inhibitors, H2 blockers, antacids
- Laxatives and antidiarrheals
- Hormonal contraceptives
- Antibiotics
In a nutshell, all the drugs mentioned above have been shown to increase intestinal permeability thus damaging the intestinal barrier. To keep things simple, remember that about 80% of your immune system resides in your gut.
Since the aim of the autoimmune Paleo diet and lifestyle is to soothe your immune system, wouldn’t it make sense to avoid anything that could irritate your gut (and hence, your immune system)?
5. If you smoke, I cannot urge you enough to quit.
Once you’ve got these factors covered, review your diet.
Are you eating your way to autoimmune diseases?
Did you know that autoimmune diseases are increasing by 2 to 10% every year?
For the skeptics out there: no, this staggering number is not solely due to better diagnostic techniques. A lot of what we eat is also contributing to autoimmune diseases by causing:
- Nutrient deficiencies
- Leaky gut (gut dysbiosis)
- Inflammation (immune activation)
To remedy to this, I suggest you start by eliminating the foods listed below.
Foods to avoid on the autoimmune Paleo diet
The following foods zap your nutrients, favor leaky gut, promote bacterial overgrowth and stimulate the immune system.
1. Grains: Wheat (including semolina and einkorn), any type of rice, barley, corn, durum, sorghum, rye, spelt, triticale, fonio, oats and Job’s tears. And of course, anything that contains gluten – check those food labels!
2. Industrial seed oils: Soybean oil, cottonseed oil, palm kernel oil, peanut oil, sunflower oil, safflower oil, corn oil and canola (rapeseed) oil.

3. Added sugars: High fructose corn syrup and anything with the word ‘syrup’ in it (like brown rice syrup), sugar and any type of sugar (such as muscovado sugar), agave, agave nectar, barley malt, caramel, dextrose, fructose, lactose, glucose, invert sugar, inulin, jaggery, molasses, treacle, sucanat.
4. Sugar alcohols: Xylitol, erythritol, mannitol and sorbitol.
5. Non-nutritive sweeteners: Aspartame, sucralose, saccharine, acesulfame K, neotame, and stevia.
6. Food additives: Olestra, acrylamides, artificial food colors, emulsifiers (guar gum, xanthan gum, lecithin, carrageenan and cellulose gum), brominated vegetable oil, propylene glycol (often added to non-alcoholic tinctures). The list is appallingly long, so I find it easier to just eat real food and avoid foods that come in boxes with a scary list of ingredients.
7. Alcohol

Once you’ve eliminated the above foods, proceed to remove the following items from your diet. These foods do NOT cause autoimmune diseases but may elicit an exaggerated immune response if you have an autoimmune condition.
1. Coffee
2. Eggs – The egg yolk may be well tolerated, but individuals with leaky guts are often sensitive to the yolks as well. As such, I recommend avoiding the whole egg if you are just getting started with the autoimmune Paleo diet.
3. High carbohydrate diets since they promote leptin resistance, inflammation and can lead to insulin resistance.
4. Legumes – Any kind of bean and peas; includes soybean and derived products like tofu, tempeh, edamame, soy isolates, soy lecithin.
5. Nuts, seeds and derived products – This includes butters, flours and oils.
6. Nightshades and derived spices – Any type of peppers (bell peppers, cayenne pepper, chili peppers), ashwagandha, cape gooseberries, garden huckleberries, goji berries, eggplant, naranjillas, paprika, pepinos, pimentos, potatoes, tamarillos, tomatillos, tomatoes. Make sure to check curry powders as these may contain nightshade ingredients.
7. Pseudo-grains – These include quinoa, amaranth, chia, buckwheat.
8. Spices derived from seeds – Anise, annatto, black caraway, celery seed, coriander, cumin, dill, fennel, fenugreek, mustard, and nutmeg.
Why exactly do you need to avoid those foods?
- Egg whites contain lysozyme, an enzyme that breaks proteins into smaller chains. Lysozyme is able to bind strongly to other proteins, including egg proteins and proteins of bacteria that normally reside in our digestive tract. Since the chemical properties of lysozyme enable it to cross the intestinal cells, any other protein attached to it will also be able to cross the gut barrier. It is those foreign proteins that prompt the body to produce antibodies. And in doing so, the body can also produce autoantibodies.
- Grains, legumes, nuts and seeds contain phytates which, when consumed in large amounts, can increase intestinal permeability.
- Allergies and sensitivities to tree nuts are very common. Since individuals with autoimmune diseases often have a leaky gut, they are more prone to developing allergies and sensitivities to tree nuts. Moreover, if you have a hidden sensitivity to tree nuts, not eliminating them will hinder your recovery rate. Plus, fibers in tree nuts can be hard to digest – this can cause sensitivities in some individuals.
- Nightshades contain glycoalkaloids (a type of saponin), lectins and capsaicin that can overstimulate the immune system and may worsen intestinal permeability in susceptible individuals.
- Legumes and pseudo-grains also contain large amounts of saponins which may be problematic for some individuals with autoimmune conditions.
Feeling overwhelmed? I know I did when I first tried the autoimmune Paleo diet. The best way to tackle it is to focus on all those foods you can eat.
Foods to include in the autoimmune Paleo diet
The following real foods are loaded with various vitamins and minerals that will help reverse any nutrient deficiency you might have.
- Meat – Beef, veal, antelope, goat, rabbit, sheep, buffalo.
- Poultry – Pastured and wild chicken, dove, duck, emu, goose, quail, turkey.
- Seafood – This includes frozen fish, canned fish in BPA-free cans and fish eggs. Besides shellfish, you might also enjoy anemones, jellyfish, sea cucumber, sea squirt, sea urchin and starfish. However, I strongly advise you to avoid fish known to have high mercury levels such as marlin, king mackerel, and tilefish.
- Offal – This includes the brain, bones, heart, kidneys, liver, spleen, sweetbreads, tail, tongue and stomach.
Note: It’s totally OK if you don’t have access, or don’t like to eat, the above foods. Just focus on a varied, high-quality diet that won’t break the bank. And if possible, go for grass-fed meat, pastured poultry, wild game, and fish.

- Vegetables – Eat as many leafy greens as you can, ideally with every meal.
- Roots, tubers and bulb vegetables such as beets, kohlrabi, lotus roots, celeriac, radish, parsnip, carrots, jicama, taro, water chestnut, sweet potatoes.
- Sea vegetables like aonori, kombu, nori, sea grape, ogonori, sea kale and sea lettuce. Avoid algae (like chlorella and spirulina) since they can stimulate your immune system.
- Fruits – Keep your fructose intake between 10 to 20 grams per day.

- Healthy fats like cold-pressed avocado oil, extra virgin coconut oil, red palm oil, extra virgin olive oil, rendered fat from poultry and cattle.
- Fermented foods like raw, unpasteurized sauerkraut, vegetables, and fruits.
With lots and lots of bone broth! Check out this video if you’re unsure how to make bone broth.
Does everyone with an autoimmune disease follow the same diet?
Actually, no – you will need to work with a qualified healthcare professional to tailor the diet to your needs and to help you with meal planning. But here are some of the modifications I recommend on a case-to-case basis:
- Psoriasis can indicate severe increased intestinal permeability – as such, limiting fruits to berries; limiting consumption of starchy veggies and maintaining normal blood sugar levels are crucial.
- Autoimmune diseases related to the HLA-B7 genes – low starch diets can be really effective in putting autoimmune symptoms in remission. But you will have to experiment with various starches (types and quantity) to determine how your body reacts the different starches.
- FODMAP-intolerance (also known as fructose malabsorption) – limiting FODMAPs (short chain carbohydrates rich in fructose molecules) can seriously improve your condition.
- Histamine sensitivity – You would need to avoid histamine-rich foods and histamine-releasing foods.
Supplements you may benefit from
- Betaine HCl if you have low stomach acid and find it hard to digest proteins. I recommend brands that include pepsin.
- Enzymes if you have digestive issues. If you’re in a lot of pain, you might also want to try taking bromelain which comes from the stem of the pineapple. Bromelain facilitates digestion when taken with meals but acts as an anti-inflammatory substance when consumed between meals.
- Ox bile if you have had your gall bladder removed or if eating dietary fats feels like you swallowed a brick.
- Glycine if you have an autoimmune disease that affects your joints, skin or connective tissues. I prefer using grass-fed gelatin and collagen powders (these have done wonders in terms of relieving my symptoms) but you can also try a glycine-containing supplement.
Glycine is involved in digestion, effective functioning of the nervous system and proper wound healing. It also helps regulate blood sugar levels and promotes muscle repair. And guess what? Glycine can help regulate both the innate and adaptive immune system!
I know how it feels to live with an autoimmune disease. And I know how intimidating the autoimmune Paleo diet can look. But if you have an autoimmune disease, I strongly encourage you to give it a try. You deserve a happy life without symptoms.